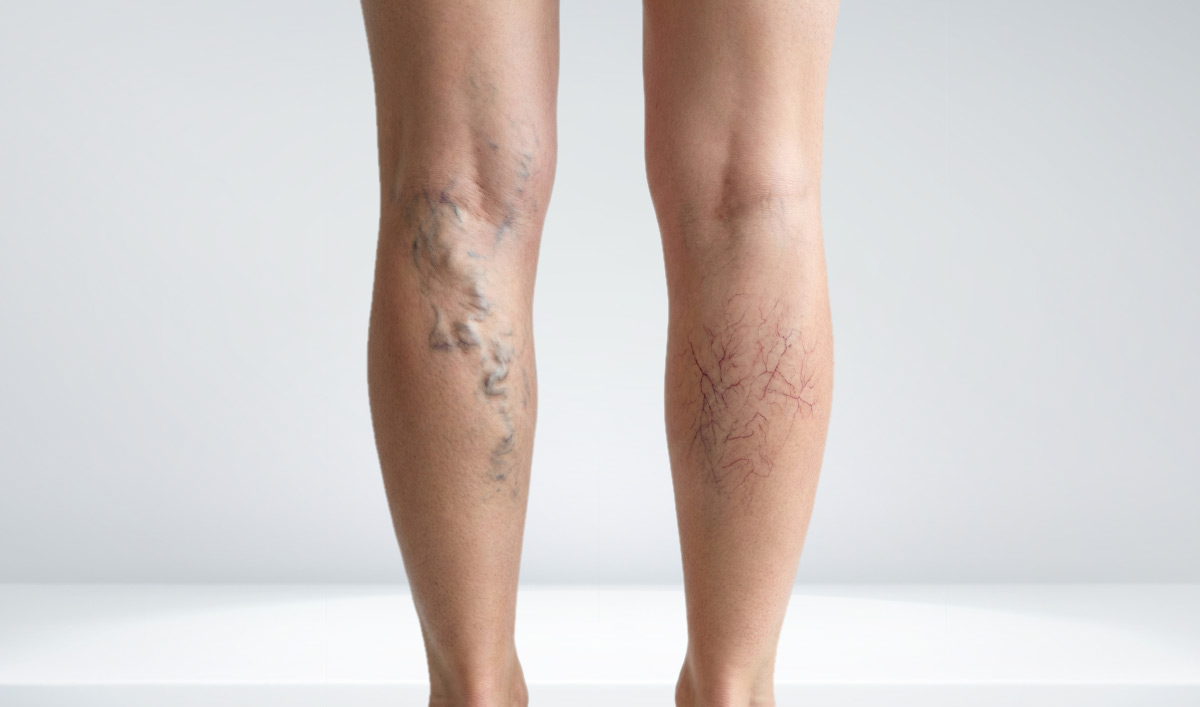
- Varicose veins are enlarged, bulging veins that can cause pain and swelling in the legs.
- Spider veins are small, superficial veins, usually a cosmetic concern.
- Both happen when the valves in your veins aren’t working properly, which causes blood to collect in your legs.
- Risk factors include genetics, hormonal changes, obesity, and prolonged periods of standing or sitting.
- Minimally invasive, safe treatments are available that allow for quick recovery.
- Ignoring persistent symptoms can allow the condition to progress, leading to chronic inflammation or even venous ulcers.
You may have noticed it when getting dressed, or after a long day when your legs feel heavy. Tiny red veins that look like a web… or bluish veins that seem to stick out more with each passing month. It’s natural to wonder: “Is this just cosmetic, or is it a circulation problem?”
At Soleil Surgical, we hear this concern every day, and we want you to know: you don’t have to get used to leg discomfort.
What Are Varicose Veins?
Varicose veins are enlarged, swollen veins that bulge visibly under the skin. They usually appear blue or purple and develop when the valves in the veins don’t work properly, causing blood to collect in the legs.
The National Heart, Lung, and Blood Institute notes that varicose veins are part of chronic venous insufficiency and can worsen if left untreated.
Many patients describe their symptoms like this:
- “My legs feel heavy at the end of the day.”
- “My ankles swell.”
- “I get nighttime leg cramps.”
If this sounds familiar, your body is sending you clear warning signs.
What Are Spider Veins?
Spider veins are small, thin veins that appear red, purple, or blue. They are flat, superficial, and usually don’t bulge or cause severe pain.
The Society for Vascular Surgery explains that while spider veins are often considered purely cosmetic, they can sometimes be linked to deeper venous insufficiency.
They may cause mild burning or fatigue, and although often just visible, in some cases they are the “tip of the iceberg.”
Why Do They Appear?
Varicose and spider veins share several risk factors:
- Family history
- Pregnancy and hormonal changes
- Jobs that require long periods of standing or sitting
- Overweight or obesity
- Aging
- Lack of physical activity
The American Vein and Lymphatic Society emphasizes that daily habits influence the progression of venous disease. Your lifestyle can either slow down or accelerate the problem.
From Diagnosis to Recovery: How We Treat Your Veins
For Varicose Veins:
- Radiofrequency Ablation (RFA): Closes the affected vein and redirects blood to healthy veins.
- Ultrasound-guided endovenous treatments.
- Compression stockings: Improve venous return and reduce symptoms.
- Lifestyle changes: Exercise and weight management.
For Spider Veins:
- Cosmetic sclerotherapy: Injection that closes the small affected vein.
- Preventive compression therapy.
At Soleil Surgical, we perform thorough evaluations, including non-invasive venous ultrasounds when needed, to check for deeper vein involvement and recommend the best treatment plan.
When Should You See a Doctor?
Schedule an appointment if you notice:
- Frequent leg pain or pressure
- Persistent swelling
- Veins that grow over time
- Changes in skin color or texture
Even if veins seem purely cosmetic, persistent symptoms often indicate a circulation issue. Over time, this can lead to permanent skin changes or venous ulcers.
The good news: when detected early, varicose and spider veins can be effectively treated with minimally invasive procedures and a quick recovery.
At Soleil Surgical, we don’t just treat veins, we treat people. We listen to your story, assess your circulation, and design a personalized plan so you can feel light, comfortable, and confident in your legs again.
Our bilingual team is here to evaluate and help you address potential risks. Don’t wait for discomfort to worsen. If you notice changes in your legs or persistent symptoms, schedule your consultation today (407) 343-4983.